What Size Hiatal Hernia Needs Surgery? It can be confusing knowing that there are many different types of hernias. You might feel puzzled if you have one and wonder if it’s a cause for concern. Hernias are common, but their various manifestations can often lead to misunderstandings.
Sometimes hernias are asymptomatic and do not require any medical intervention and sometimes they can cause issues that jeopardize your health. How do you know what size hiatal hernia needs surgery? Is it the size or location that determines the need for surgery vs. taking the watchful-waiting approach?
Today, we will discuss hernias, the distinctions between a medium-sized hiatal hernia and a moderate-sized hiatal hernia, how to identify hernia symptoms, and when to perform hernia surgery.
Why Does a Hernia Occur?
Muscles and tissue are key elements that hold your organs in place. Sometimes, the breakdown of muscles and tissue can weaken an area, and it can cause an organ to push through that weak spot, protruding into an area where it does not belong. We call this condition a hernia, and it typically develops in the region between the chest and the hips. It often manifests as a visible bulge or lump on the abdomen or groin. It can frequently appear as a visible bulge or lump on the abdomen or groin.
Some hernias are located internally and will not be visibly noticeable from outside the body. Although, we call these hiatal hernias, and they may come with symptoms or may not cause any symptoms at all.
What Types Of Hernias Can Occur?
The most common hernias that an individual may experience include:
Inguinal
A hernia that forms on the inner groin.
Femoral Hernia
A hernia that forms on the outer groin.
Incisional Hernia
A hernia that forms in the area of a previous surgical incision.
Umbilical Hernia
A hernia on or close to the belly button:
Hiatal Hernia
An internal hernias form in the upper portion of the stomach. There are two types of hiatal hernias:
Sliding Hernia
A sliding hiatal hernia occurs when some of the stomach and the point where the esophagus connects to the stomach slide and shift upward into the chest through the connection point of the diaphragm and the esophagus (the hiatus).
Paraesophageal Hernia
A larger sliding hernia that involves a bigger portion of the stomach and sometimes other organs protruding through the hiatus.
What Symptoms Do Hiatal Hernias Cause?
Sliding hiatal hernias are fairly common and 1 out of 4 adults experience one by the time they are 40 years old. When one occurs, they can often cause chronic GERD.
Paraesophageal hernias are less common but they can be more concerning. However, in some patients, doctors can simply monitor the hernia without taking any medical action. Other patients may experience symptoms and are at a higher risk of developing an incarceration situation. When this happens, a portion of the stomach that is protruding through the opening becomes stuck cutting off the stomach’s blood supply and resulting in the need for emergency surgery.
All hiatal hernias are associated with the development of Gastroesophageal Reflux Disease Symptoms (GERD). Patients usually first try to make changes to their lifestyle such as not eating too late at night, sleeping propped up on pillows, taking medications that help reduce stomach acid, etc.
Overall, experts feel that symptomatic Paraesophageal Hernias should be repaired to alleviate the escalation of symptoms to emergency status.
Common Symptoms of a Paraesophageal Hernia
1. Chest Pain
There can be many causes for chest pain but patients that have a known paraesophageal hernia that is large should have a cardiac evaluation to ensure the pain is not related to their heart. Many patients with a paraesophageal hernia have general pain after every meal and others experience pain intermittently. Other symptoms occurring at mealtime may include:
- Difficulty with swallowing.
- Abdominal pain (located in the upper or middle abdominal region).
- When eating, the person becomes “full” abnormally quickly and remains feeling full for an abnormally long time.
2. Shortness of Breath
The patient may easily become short of breath. Some very large Paraesophageal Hernias cause the stomach to push on the diaphragm or put pressure on the lungs causing the feeling of not being able to take a deep breath.
3. Stomach Ulcers
Some patients may experience a rare occurrence of the stomach twisting upon itself and creating a stomach ulcer called Cameron’s Erosion which can sometimes cause life-threatening bleeding.
This can facilitate gradual blood loss and result in a condition called anemia. Anemia occurs when your body is not able to produce enough healthy red blood cells to carry and supply oxygen to all the tissues and organs that need it. Anemia causes numerous symptoms such as extreme fatigue, weakness, dizziness, shortness of breath, chest pain, cold extremities, headaches, etc.
Many individuals with Paraesophageal Hernias also suffer from GERD (gastroesophageal reflux disease).
Hiatal Hernia Classifications
Hiatal hernias can form in different sizes with a smaller hernia being about 2-3 cm in size, and a medium size hiatal hernia ranging from 4-5 cm. Once the hernia becomes 5 cm+ it is considered a large hernia. The type of treatment required for a hiatal hernia depends upon how advanced the hernia is. Hiatal hernias are classified from 1 to 4 by how severe they protrude into the esophageal hiatus.
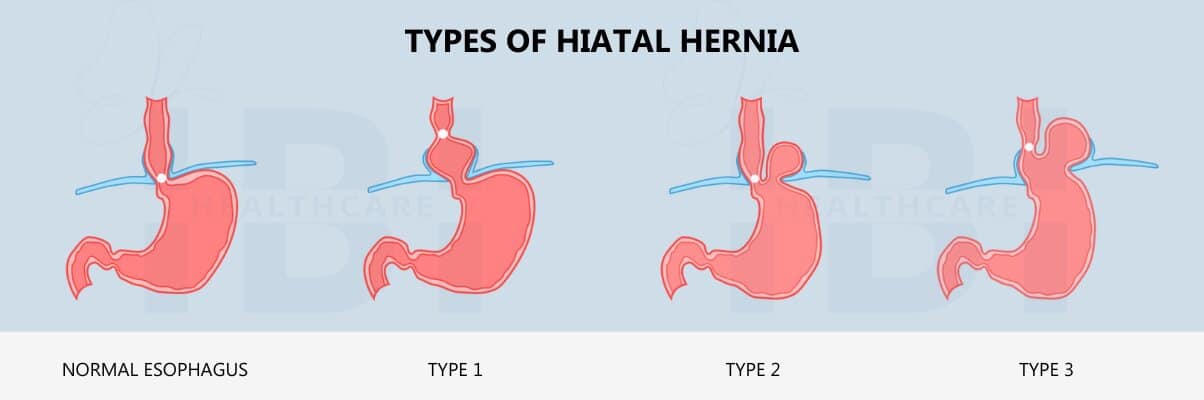
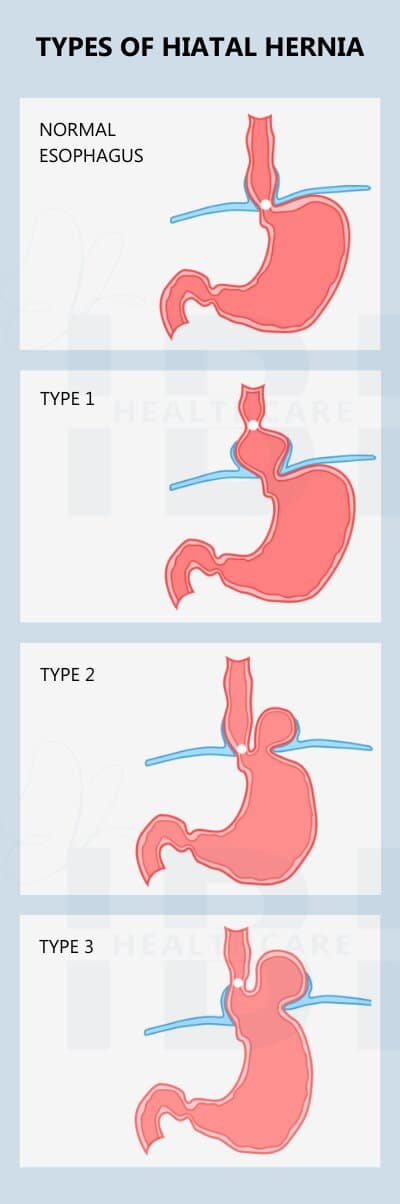
- Type 1 or sliding hiatal hernia is the most common type of hiatal hernia and is also one of the hardest to diagnose. Reflux is one of the earliest symptoms and may be the only indication of type 1 hiatal hernia.
- Type 2 – occurs when the top portion (fundus) of the stomach pushes through the esophageal hiatus but the connection point (GEJ) between the stomach and the esophagus remains below the diaphragm.
- Type 3 – Once a hernia progresses into the type 2 category, the possibility of mechanical complications increases. Now that the esophageal hiatus has been compromised, the widening of the opening can become increasingly worse, and allow more of the stomach tissue to enter the hiatus. In a type 3 hernia, the GEJ shifts to a position above the diaphragm, and more of the stomach protrudes into the chest area.
- Type 4 – This type of hernia occurs when the stomach and other organs such as the pancreas, colon, spleen, etc., enter the chest cavity. This happens due to the stretched-out opening as well as a defect in the pharyngoesophageal membrane which is designed to hold the esophagus in place.
Types 2-4 are variations of Paraesophageal Hernias and represent between 5% and 15% of hiatal hernias.
How Are Hiatal Hernias Repaired?
The treatment of a hiatal hernia will vary according to the associated symptoms.
- Doctors typically manage mild hiatal hernias (type 1) with reflux medication, and they do not require any special treatment.
- If type 2 or 3 hernias become symptomatic they usually require surgery.
- Type 4 hiatal hernias will require surgery.
Hernias are most often repaired laparoscopically. The overseeing doctor can help determine when and what type of surgery will benefit your condition.
1. Laparoscopic Repair
During laparoscopic hiatal hernia repair, surgeons create about five very small incisions in the abdomen and use them to manipulate the protruding portion of the stomach back to its correct location.
Furthermore, surgeons close the diaphragm (at the junction of the esophageal hiatus) to prevent the stomach from slipping back through. In specific cases, surgeons wrap the fundus (the top portion of the stomach) with a mesh-type material to ensure they properly close the diaphragm, thereby preventing the stomach from re-entering the chest cavity.
Most people who have laparoscopic hernia surgery can return home the same day. Sometimes a hospital stay may be required for those who undergo abdominal wall reconstruction or other more involved repairs.
2. Open Hernia Surgery
Sometimes patients are not eligible for laparoscopic surgery and require open hernia surgery. The surgeon creates a large incision in the abdomen and moves the stomach back to where it belongs. Also, wrap the fundus with a special surgical mesh to prevent the stomach from moving again.
Sometimes a temporary tube is inserted to help keep the stomach in place during healing.
What Size Hiatal Hernia Needs Surgery?
In most cases, hernias will eventually grow larger and can lead to serious complications if people do not repair them.
Typically, individuals can self-manage hernias that are smaller than 5 cm (2 1/2 inches) through lifestyle choices and medication. Most problems patients experience are linked to large or moderate-size hiatal hernias.
Researchers conducted a study that examined 192 patients with both large and small hiatal hernias and reflux. The aim was to determine if the size of a hiatal hernia (large or small) played a role in the intensity of the reflux they experienced.
Researchers monitored the patient’s PH levels when they were lying down and sitting up. The hernias were considered small if they were in the range of 2 to 4 cm and large if they were 5 cm or larger.
The intensity and length of the pain and symptoms of reflux were directly related to the size of their hiatal hernia. The longer and more frequently they experienced these symptoms, the more prevalent the esophageal erosion. The symptoms for patients with hiatal hernias that were 5 cm and over were twice that of patients with smaller hernias.
Can You Fix Any Hiatal Hernia Size At Home?
Hiatal hernias do not repair themselves but there are some things patients can do to minimize their symptoms. Moreover, the smaller the hernia, the more chance you can manage the symptoms at home. Symptoms can sometimes be managed through:
Medications
Over-the-counter remedies such as antacids can sometimes provide quick relief but these can cause kidney issues if used long-term. People know H-2 receptor blockers like Tagamet HB and Pepcid AC, or medications that block the production of stomach acid such as Prevacid 24HR, as proton pump inhibitors, and they consider them stronger than H-2 receptor blockers.
Exercise
Maintaining a healthy weight and engaging in a consistent exercise routine.
Lifestyle Changes
- Stop smoking.
- Avoid eating late in the day.
- Sleep in a reclined position.
- Eating several small meals during the day instead of 1 or 2 large meals.
- Avoiding food that triggers reflux and heartburn like fried foods, and acidic, and fatty foods.
If you feel you may have a hiatal hernia, it is important to have it checked out by a qualified professional. People must manage hernias through lifestyle changes and/or surgical repair because hernias will not repair themselves and will continue to worsen. Nevertheless, contact IBI Healthcare Institute to set up a consultation. The qualified professionals at IBI Healthcare Institute can perform hernia repair surgery and bring you relief from painful hernia symptoms.
Lastly, if you’re experiencing heartburn and acid reflux symptoms and triggers. Check our free Online GERD Calculator to determine your GERD score and stage.









